The rise of non-communicable diseases in Africa adds to COVID-19 stress
The COVID-19 pandemic in 2020 has highlighted Africa’s vulnerability to disease in an unprecedented manner, laying bare years of under investment in public health facilities and systems. As infection rates ratcheted up across the world, African governments scrambled to patch up dilapidated public infrastructure and build capacity to prepare for an expected tide of coronavirus patients. The fear among international analysts and observers was that Africa would be far worse hit than many other regions because of its fragile health systems and its high disease burden, which made Africans more vulnerable to infection and possible fatalities linked to the virus. While Africa accounts for less than 2% of global health expenditure, it carries 26% of the disease burden, according to the UN Economic Commission for Africa’s 2019 report, Healthcare and Economic Growth in Africa, with hundreds of thousands of deaths each year from a range of illnesses such as malaria, HIV/Aids and tuberculosis (TB).

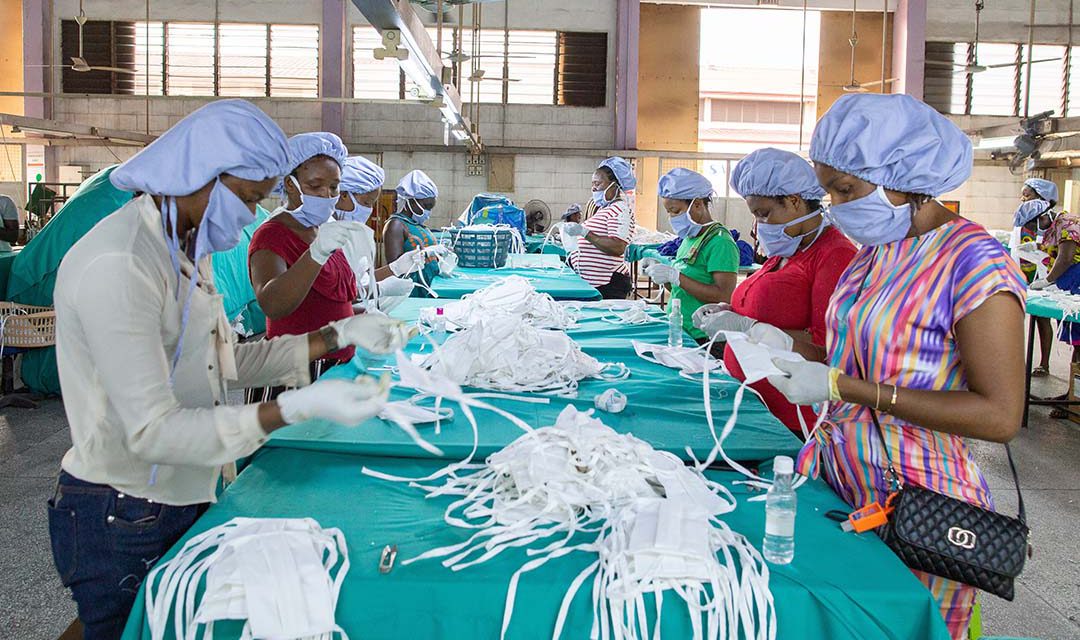
Factory workers check personal protective equipment for COVID-19 frontline health workers at a factory commissioned by the government in Accra, Ghana, April 2020. Photo: Nipah Dennis/AFP
At the early stage of the pandemic, COVID-19 modelling suggested that the virus could claim more than three million lives in Africa. International medical journal The Lancet said at least 283 million of Africa’s 1.3 billion population was at a high risk of severe COVID-19 because of underlying health conditions. Five months into the pandemic, by mid-August, the number of COVID-19 cases in Africa was just over a million and about 26,000 people had died from complications linked to the virus. Dr John Nkengasong, head of the Africa Centres for Disease Control, when asked about the predictions, said, “The worst-case scenario is where nothing is done and a continent of 1.3 billion is infected. But something is being done.” But global health experts maintain the true toll is probably much higher given low testing rates. The ACDC said in July that by then the whole continent had carried out a total of 7.2 million tests and 80% of them were conducted in only 10 countries and of these, mostly in one – South Africa.
On the other hand, experts in the medical field point to Africa’s experience in dealing with health emergencies, citing their experience in dealing with infectious diseases. Nigeria was dealing with an outbreak of Lassa fever when COVID-19 landed earlier this year. Countries such as Democratic Republic of Congo (DRC) affected by the Ebola virus have developed systems to respond to highly contagious epidemics. Many also point to Africa’s high youth population, a segment believed to be less at risk from the virus, and the fact that 60% of people live in rural areas and may have escaped contact with infected people. The concerns about the impact of COVID-19 on Africa is related to its high incidence of diseases that present co-morbidities for the virus and that increase the potential for higher fatalities. These include malaria – Africa has more than half of all cases globally – as well as infectious diseases such as tuberculosis (TB) and HIV.
In 2018, more than 1.5 million Africans died from TB, including 251,000 who also had HIV. South Africa has the highest number of TB infections and HIV prevalence in the world at 20% of the population. Malnutrition is already a key driver of sub-Saharan Africa’s disease burden. The UN World Food Program says more than 820 million people regularly go to bed hungry. The COVID-19 pandemic could now double that number by the end of 2020. As it tackles the “old” diseases, Africa faces new health challenges with the dramatic rise of noncommunicable diseases (NCDs) such as diabetes, obesity and hypertension, which now account for a hefty 37% of the disease burden. The Lancet medical journal says that as health systems in sub-Saharan Africa are largely focused on tackling infectious diseases and maternal, neonatal and child deaths, they are paying insufficient attention to the region’s ‘rapid epidemiological transition’ – the shift from communicable diseases such as malaria, TB and HIV to NCDs.
Research indicates a growing burden of diabetes, chronic respiratory and kidney diseases, cancer and cardiovascular problems, driven by tobacco consumption, harmful alcohol use, unhealthy diets, physical inactivity, obesity, or high blood pressure. Diabetes has been identified as the most serious comorbidity with COVID-19. Professor Joel Dave, head of endocrinology at the University of Cape Town, has estimated that 42% of people hospitalised for COVID-19 in South Africa’s Western Cape province, who also had diabetes, had died as of mid-July. The risk of death in this instance rises from four times for patients on treatment for diabetes to 13 times for those on no treatment. The condition is particularly dangerous because many people are unaware of they have it. “Accurate current data on the prevalence of diabetes in South Africa is quite difficult to find as there are no recent robust studies done in all provinces,” Dave said. The International Diabetes Federation, in its 2019 report, puts the number of adults in Africa living with diabetes but unaware of it at a high 60%, which is why it is often referred to as the silent killer.
The Federation says the current number of 19 million adults in Africa living with the condition is expected to increase to 47 million by 2045. In South Africa, the incidence of the disease rose by 137% between 2017 and 2019. Doctors in South Africa predict that the incidence of both old and new diseases will increase in the wake of COVID-19 due to the failure of hundreds of people to maintain treatment schedules or access chronic medication because of the country’s strict lockdown. This has also affected diagnosis of diseases other than COVID-19, a situation likely to be replicated in other countries that imposed lockdowns. The pandemic has also exposed the poor state of public facilities, not just in urban areas but across the continent, with healthcare at district levels appears to be in a particularly parlous state. The continent has just one hospital per one million people, and one doctor and one hospital bed per 10,000 people, according to the World Health Organization (WHO).
Governments cite resource limitations when defending their record in the sector. Only a handful of countries have met the African Union’s 2001 guidelines to allocate 15% of their budgets to health, with average expenditure in the 5-6% range. According to the UN’s Economic Commission for Africa (ECA), a third of countries have reduced health spending, often relying on donors to fill the gap. But money is just one part of the problem. Others include poor leadership in the public sector, wasteful expenditure, inefficient supply chains and a lack of skilled health professionals. These contribute to the poor outcomes for money spent, which militate against higher spending as the only solution to the challenges. The funding gap for health is large and new financing options are limited given the dent the pandemic has made in growth rate predictions in Africa and elsewhere. The African Development Bank estimates that COVID-19 could cost Africa a GDP loss of between $22.1 billion and $88.3 billion in the worst-case scenario.
Depending on the trajectory of the virus, the continent could fall into recession by the year end. Nevertheless countries have options, including building stronger public-private partnerships to attract investment into the sector. ECA Executive Secretary Vera Songwe says Africa should invest in its pharmaceutical industry. The continent currently imports more than 70% of its needs, a market worth about $14 billion, she says. Meanwhile, the World Economic Forum suggests that a greater focus on building digital solutions to longstanding healthcare challenges will make African systems more efficient, with mobile technology and broadband being the building blocks of reform. Already, African entrepreneurs have devised digital solutions to issues of data capture, remote diagnosis and testing and information sharing. COVID-19 offers the continent a chance for a reset; a fresh look at its intractable problems. Building a more resilient health sector is vital, not just for managing this and other possible pandemics, but to enable the continent to tackle its double health burden of communicable diseases and the rising tide of NCDs.
The real test of whether anything has been learned from the pandemic will be when the dust settles. Will it be a return to normal, where the healthcare sector once again takes a back seat to other political priorities, or will Africa’s health systems emerge more robust and efficient as a result of the increased attention paid to training staff and improving facilities, among other interventions? Dr Matshidiso Moeti, head of the WHO Regional Office for Africa, says Africa’s success in bringing down deaths from malaria and HIV/AIDS has been due to greater political commitment, strong global partnerships, increased financing and more effective interventions. These same factors need to be applied in tackling NCDs and malnutrition in Africa. A mind shift change needs to accompany wider reforms, with policymakers encouraged to view health expenditure as an investment in the sustainability and transformation of their economies rather than a drag on government revenues.
Dianna Games is a leading commentator on business trends and developments
in Africa. She is the author of many published reports on African business and is
a columnist on Africa for Business Day newspaper in South Africa and African
Business magazine in the UK. She also heads the SA-Nigeria business chamber.