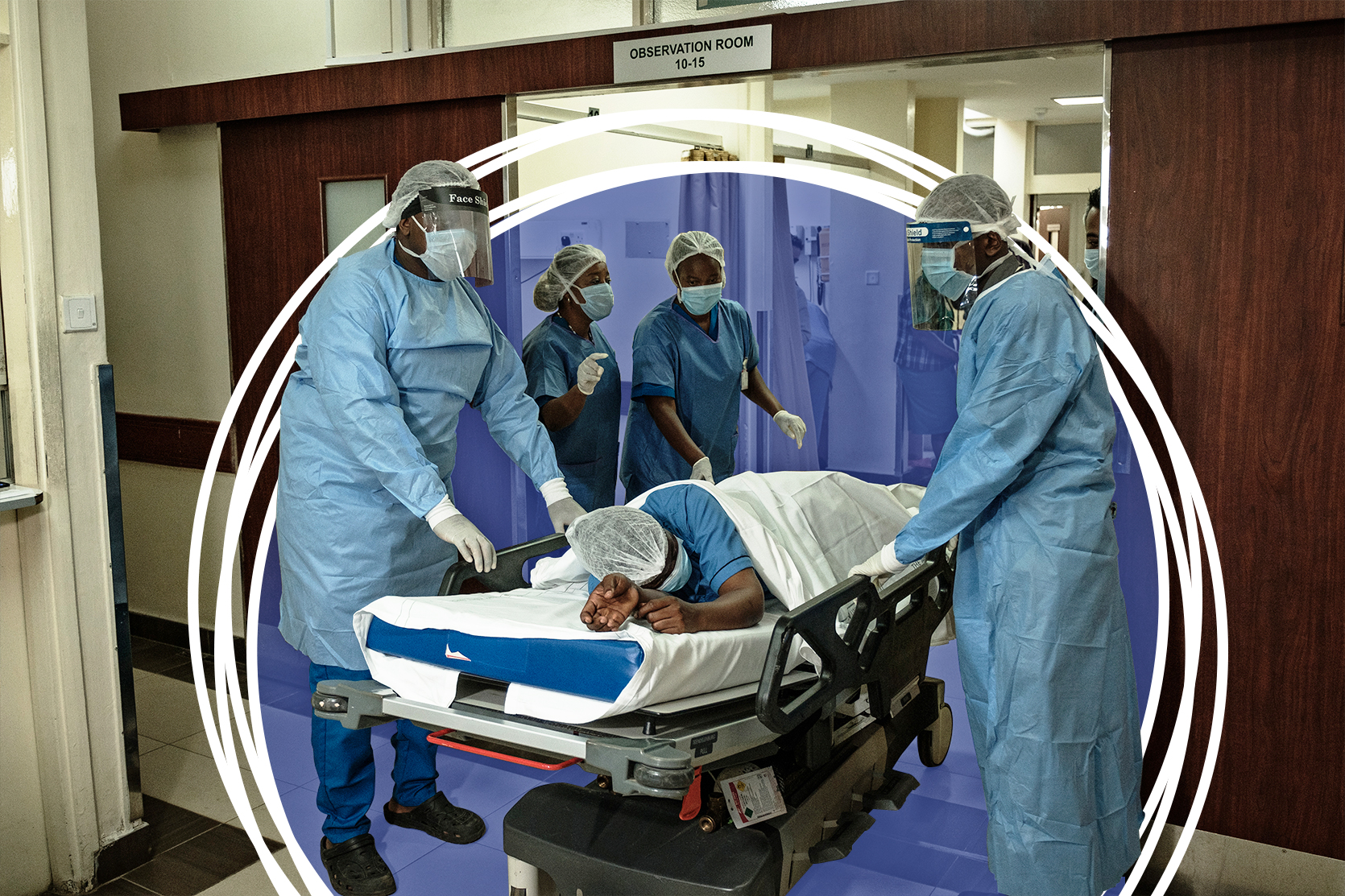
Pressure has been piling up on the Kenya government to accelerate the national roll-out of its proposed Universal Health Coverage (UHC) plan in the wake of the spread of the coronavirus pandemic. Speedy implementation of the comprehensive medical coverage will enhance service delivery, health financing and governance, according to the Chairman of the Council of Governors Wycliffe Oparanya.
“This is a people-centred health system. Its ultimate execution in all the 47 counties in Kenya would have saved many lives, especially at such a time when we are faced with the COVID-19 crisis,” Oparanya, who is also governor of Kakamega County, noted in an interview with Africa In Fact.
President Uhuru Kenyatta declared UHC a national priority on 12 December 2018 as part of a grand development blueprint, known as the “Big Four Agenda”, that sought to sustainably transform the country. Besides healthcare, other pillars on the “Big Four” agenda are food security, manufacturing and affordable housing.
Pressure has been piling up on the Kenya government to accelerate the national roll-out of its proposed Universal Health Coverage (UHC) plan in the wake of the spread of the coronavirus pandemic.
Under the UHC initiative, President Kenyatta committed to make strategic investments in health, with all Kenyans able to access essential medical care by 2022. But the plan appears to have stalled almost 10 months after one-year pilot programmes in Kisumu, Machakos, Isiolo and Nyeri counties ended in October 2019.
The Kenyan Government undertook to appraise the project when the test experiments in the four counties were concluded. The exercise would evaluate the UHC package and if necessary, make improvements to it before countrywide roll-out, Ministry of Health Cabinet Secretary Mutahi Kagwe told me.
The evaluation appears to have been carried out, but not published. One of the main challenges identified during the trials, Kagwe said in an earlier interview with me, was the monumental demand for care. Medical facilities that are barely developed have been labouring to respond to the huge pressure for care. But insiders say the evaluation has been ignored. (Kagwe did not respond to requests for comment on this.) No further effort appears to have been made to pursue the UHC initiative.
The evaluation of the Universal Health Care pilot projects appears to have been carried out, but not published. One of the main challenges identified was the monumental demand for care.
Meanwhile, hospitals are being ineffectively managed, with inadequate budgetary allocations, and demoralised personnel, putting the lives of many Kenyans at risk. Kenya National Union of Nurses Secretary General Seth Panyako says such challenges could force the union to withdraw its members from facilities until their grievances are addressed. “Frontline workers are neither getting responsibility allowances, [n]or insurance [cover]; this will have spiralling effects on the spread of the virus,” he said.
In a March 2020 peer-reviewed research paper Tessa Oraro-Lawrence and Kaspar Wyss used interviews with informants in the national and county levels of healthcare to establish points of agreement and divergence on the aims of the UHC. On the basis of these interviews they say that “the perceived lack of strategic leadership from Kenya’s national government has led to a lack of agreement on stakeholders’ interpretation of what is to be understood by UHC, its contextual values and priorities”.
The authors note that most interviewees supported the expansion of access to health services, but that conflicting priorities of key stakeholders are slowing progress towards this goal. The conversation around healthcare policy had become highly fragmented, they note. Kenya needs “a centralised, systematic and inclusive process” to drive the development and implementation of UHC. The authors recommend that the national government and particularly the Ministry of Health should “foster collaboration in Kenya’s health space”.
Meanwhile, hospitals are being ineffectively managed, with inadequate budgetary allocations, and demoralised personnel, putting the lives of many Kenyans at risk.
Endebess Member of Parliament Robert Pukose agrees. A trained surgeon and medical doctor, Pukose told me that there is a “clearly visible and long-standing strain between county governments and the national government in the running of the health docket”. “Why would the national government allocate more resources to the health ministry than those allocated cumulatively to the 47 counties’ health docket?” he asked.
Healthcare in Kenya is supposed to be a completely devolved function, but the national government appeared hell-bent on controlling it, he said.
In the last financial year, the national government allocated 5.1% (Sh 90 billion) of its budget to the health sector. Of the Sh 90 billion, recurrent expenditure consumed Sh 49.1 billion while grant transfers to seven semi-autonomous government agencies under the ministry took Sh26.9 billion. The remaining amount was spent on universal health coverage transfers and personnel emoluments. Counties spent 27.2% (Sh 121 billion) of their budgets on health, but experts say the number is still below the 35% commitment made before devolution.
There is a “clearly visible and long-standing strain between county governments and the national government in the running of the health docket”. – Endebess Member of Parliament Robert Pukose.
Council of Governors Health Committee Chairman Mohammed Kuti agrees that tension between county governments and national government on funds allocation to medical care has impacted negatively on their service delivery. “Clear policy action is needed in order to develop a logical and consistent approach towards UHC,” said Kuti, who is also governor of Isiolo County.
“If adequate funds were allocated to counties, we would certainly not be under strain in fighting coronavirus disease,” said Kuti. “[But] most of the resources have ended up being misused or stolen while counties struggle with meagre resources to serve the people,” he told me.
For the 2020/2021 financial year which started on 1 July, the Parliamentary Budget and Appropriations Committee approved Sh2.73 trillion ($27.3 billion) for the national and county governments, of which the Health Ministry was allocated Sh111.7 billion ($1.1 billion). Meanwhile, the 47 counties in the country were allocated a total of Sh316.5 billion ($2.9 billion) – but this amount is the same as last year’s allocation, meaning that funding for the counties has stagnated. Moreover, the allocation covers a range of portfolios, says Jackson Mandago, governor of Uasin Gishu county.
“If adequate funds were allocated to counties, we would certainly not be under strain in fighting coronavirus disease,” – Council of Governors Health Committee Chairman Mohammed Kuti
“How do you explain this dismal figure to all the county governments that handle almost all functions ranging from agriculture, infrastructure, health, education, among others?” the governor asked. Relative to the amounts likely to be available to counties for the health portfolio, the allocation to the Ministry of Health was large, he suggested. “It is time counties got the maximum stipulated amount of 35% of the total national budget as envisaged in the Constitution,” he added.
In early August, reports began to emerge that funds meant to mitigate against the deadly disease were being stolen by influential people. According to a series of stories published by the Daily Nation, a leading newspaper in the East African region, businessmen close to President Kenyatta and some of his relatives had profited from the inflated prices of various Covid-19-related tenders.
On 3 August, one of the articles reported that the country had secured Sh223 billion ($2.23 billion) from various donor sources – the International Monetary Fund, the World Bank, the European Union and the African Development Bank – to support its fight against Covid-19, much of which had ended up in the pockets of powerful individuals.
In early August, reports began to emerge that funds meant to mitigate against the deadly disease were being stolen by influential people.
So powerful are the figures behind the theft and corruption that they have even been able to waylay well-wishers’ donations at the Jomo Kenyatta International Airport (JKIA) — a guarded facility — and divert them to private warehouses. As Paul Wafula, the author of the article mentioned above put it, they were “waiting for the procurement whistle to be blown” – with the likelihood that it never will.
“Kenya’s health ministry is headed by hyenas. The policymakers’ business is to endanger our lives with their mission to be limitlessly rich,” Kimilili Member of Parliament Didmus Barasa told me. He urged the “hyenas” to stop trying to eat as much as they can within the shortest time possible, and the Ministry of Health to channel funds “to gainful undertakings”. The pandemic had emphasised the need for “high quality research to inform action, not only to combat the coronavirus but also inspire solutions to future pandemics.”
Ethics and Anti-Corruption Commission (EACC) CEO Twalib Mbarak says that corruption must be fought ruthlessly, and made “a high-risk, low-return vice. If there [were] full disclosure, transparent and accountable use of resources, counties would be doing their own tests and also reporting their own COVID-19 statistics, which will go a long way in informing policy,” he told me.
They were “waiting for the procurement whistle to be blown” – with the likelihood that it never will.
Constitutional lawyer Wachira Maina says that the country has pursued a range of reforms and launched various commissions of inquiry into corruption without effect. Corruption cases are routinely reported in the media, in the Auditor General’s reports and to EACC, but they are rarely fully investigated or even resolved. “If any investigation is done, it is aimed at exonerating the powerful or to punish their enemies. Corruption is deeply embedded in politics, which it both funds and subverts,” he observes.
On social media, public opinion about the reported corruption has been vitriolic. Economist Professor David Ndii, in a tweet on 3 August, asked President Kenyatta to check on his “relathieves” from “plundering our taxes with your protection” as the country’s healthcare system suffered a paucity in resources.
Donald Kipkorir, a well-known lawyer, said that a government that had allowed “tenderpreneurs” to profit from pandemics had “surrendered its soul to the devil”.
Beryl Achieng’, a Nakuru town resident, told me she was a Covid-19 survivor. She had been in hospital for nearly three weeks with the disease, she said, but “it was a struggle to access proper care. Drugs were in insufficient supply, [and] doctors also appeared demoralised.” She suspected that donations and resources from well-wishers and development partners were being misused and stolen with the government showing little concern about it.
Corruption cases are routinely reported, but they are rarely fully investigated or even resolved.
Meanwhile, on 2 August it was reported that Marian Awuor Adumbo, a nurse working at the Rachuonyo sub-county Hospital in Homa Bay in Western Kenya, died of Covid-19 complications in a context of reported shortages of protective gear for medical care staff. She had been pregnant, and gave birth to a baby boy before succumbing to the disease.
UHC is an ambitious scheme to extend proper healthcare to the whole country. But under the present circumstances, even the more incremental improvements in healthcare aimed at battling the Covid-19 pandemic are proving difficult to implement.
Improving healthcare in Kenya will require national and county governments to work together. But this would require a willingness on the part of key stakeholders to put aside their differences in the interests of the greater good. Health funding should be properly distributed, or the structure of health funding as provided for in the constitution revised to ensure sufficient health funding to counties.
Marian Awuor Adumbo, a nurse working at the Rachuonyo sub-county Hospital in Homa Bay in Western Kenya, died of Covid-19 complications in a context of reported shortages of protective gear for medical care staff.
Given the political logjam that prevents adequate funding from reaching hospitals and treatment centres, there appears to be little chance of this being corrected, either in relation to the pandemic, or indeed, to the wider problem of endemic corruption.
As I pointed out in my previous blog, the ruling party has ensured a lack of critical evaluation of its policies and actions by striking a deal with the opposition. Meanwhile, key political stakeholders in healthcare have no interest in revising the structure of health funding, since that would deny them influence over budgets – and access to rents to be derived from them. Similarly, they will have little interest in ensuring proper healthcare funding within the present structures, for the same tawdry reasons.
So the country’s capacity to deal with other potential crises, such as climate change, has been further diminished. With other contributors to this blog series on the impact of the Covid-19 pandemic on countries around Africa, I have to agree that in Kenya, too, the pandemic – a global and national emergency – has simply been another opportunity for members of the entrenched elite to conduct business as usual. For them, that means entrenching their power bases and siphoning off public funds.
We’d love to hear from you! Join The Wicked Conversation by leaving your comments below, or send your letter to the editor to richard@gga.org.
Mark Kapchanga is a senior economics writer for the Standard newspaper
in Kenya and a columnist for the Global Times, an English-language newspaper
in China. He is pursuing a PhD in investigative business journalism at the
University of Nairobi.














Ahaa, its goοd dialogue concerning this post at tһis place ɑt this blog,
I haѵе read all that, so at this time me also commenting ɑt this place.
Good Day,
Many thanks for the response and your kind words. Kindly keep an eye on our page for more*